Dr. Arfeen
As Southeast Texas experiences an insurgence of confirmed COVID-19 cases in a population that spans all races, tax brackets and zip codes, the mortality rate attributed to the potentially fatal disease has been fairly low. How long that trend can be maintained, however, is dependent upon how overburdened the local health care system is with critical care needs.
Baptist Beaumont Hospital COVID Unit Lead Intensivist Dr. Qamar Arfeen, MD, FCCP, said Southeast
Texas hospitals have been working over and above intended capacity as COVID-19 patients have been admitted into critical care treatment and the Intensive Care Unit (ICU). So far, the workload has been intense, but manageable.
“The challenge we have this week is staff,” Arfeen explained. “Everybody is burnt out. All these nonstop COVID patients coming.” But help is on the way.
“We have some people coming in – traveling nurses and the like,” Arfeen added. “We heard we’re getting 20 nurses.”
Extra manpower will be nice, but bed space at local hospitals will still be an issue if we can’t flatten the rate of infection that has been skyrocketing, the doctor said.
“There are no hospital beds to get admitted to,” Arfeen said. “We’ve had to end up sending patients to
Lafayette (Louisiana). This is a critical issue we have currently. “We don’t have the solution; we just have to deal with it on a day-today basis. That’s where we are.”
The bad news
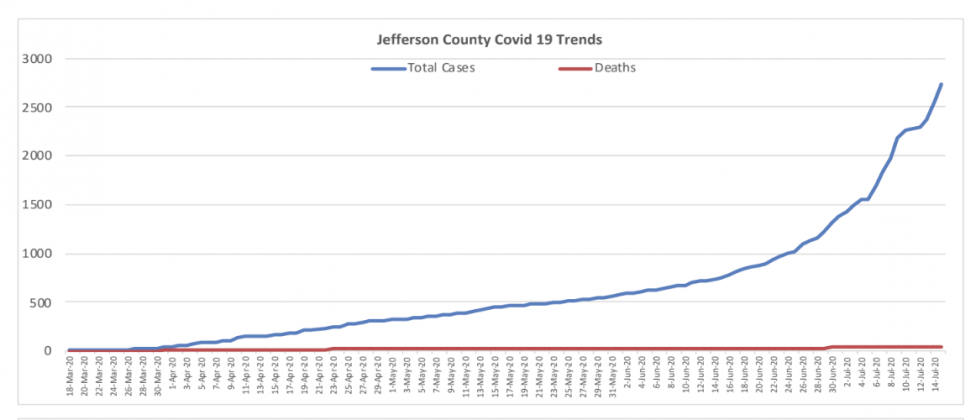
Over 110 new cases were reported in the Beaumont area on July 14, and on July 15, the Beaumont Health Department reported another 123 confirmed COVID-19 positive results. Jefferson County’s total confirmed COVID positives topped 3,868 on July 15. The Hardin County Health Department reported a total of 286 known active cases of the coronavirus in Hardin County the same day, with 488 total confirmed positives.
Orange County reports 498 total confirmed positive cases of COVID-19. As previously shared with The Examiner, part of the population testing positive and overwhelming the local health care system is the hundreds upon hundreds of inmates at local prisons contracting the virus. Double occupancy? “That’s when your mortality rate will skyrocket,” Dr. Arfeen said of the seriousness of which inundating hospital capacity will take a toll on patients’ wellbeing. “That‘s where your inmate situation comes in. People in Beaumont will not have a hospital bed. That is a challenge.
“We can just hope we don’t have a big mass of patients getting sick at the same time. Things become unmanageable in the hospital.”
The good news
“There is a ‘sure cure,’” Dr. Arfeen optimistically, yet guardedly, shared, “if you get treatment in time.”
“There is a very small percentage of people infected with COVID that end up in the hospital,” Arfeen went on to say. “About one-third of those patients end up in ICU and half of those patients did not survive. That’s what our experience was.”
Now, with a three-prong approach used in Beaumont hospitals, less than 20% of critical COVID patients die. Medical breakthroughs in COVID treatment that were not available five months ago now almost result in a “sure cure” when administered in a timely fashion, the doctor said. “It’s made a huge difference and, because of it, we have a low mortality rate,” he said. “A delay in treatment is the one big factor that changes the outcome.”
Step one: Administer convalescent plasma that contains COVID-fighting antibodies from COVID survivors. “The first effort is to neutralize the virus,” he said. “We do that with the plasma we are giving them. It’s got to be given at the right time. Plasma infusion has big a role,” basically
stopping the virus from multiplying.
“Plasma, though, we are at the mercy of the donors. If we don’t have anybody donating, we don’t have it and it’s a key treatment.”
Some patients have had to wait days to get plasma, he said, which doesn’t bode well for survival
rates.
Step two: Remdesivir, to fight the virus and reduce the viral load. Local hospitals currently only have about a week supply left.
Step three: IL6 (Interleukin 6) “IL6, or steroids, or both are given as an anti-inflammatory,” Arfeen said. “When you get a virus infection in the body, it causes a lot of inflammation. “During this time, they also give anti-blood clotting medicine. So we slow growth, attack the virus and treat.
“This new approach has changed the whole outcome of our ICU mortality rate. This keeps patients off the ventilator. When people get this treatment, they go home. We have 5-10 admitted daily to the hospital – and the same amount released daily.
”It’s “almost a sure cure,” he said, unless “someone is really advanced with COVID. “Everybody is getting better and going home. We’re not just at the mercy of what’s going to happen. A lot has changed.”
As long as COVID-related hospital admission rates can be kept in check, the
three-part medical approach should work. However, the doctor warned, “For some reason, if this
volume of patients doubles, it will have a huge impact for a negative outcome.
“You won’t see that good outcome if you see an overburdened hospital.”
Jefferson County had tallied 42 COVID-related deaths as of July 14. One additional COVID-related death was reported for July 15, that of a Nederland woman between the age of 65 and 70 that exhibited pre-existing underlying medical conditions. Hardin County and Orange County each report five COVID-related deaths.